1-855-452-6224 (Customer Support Available 24/7)
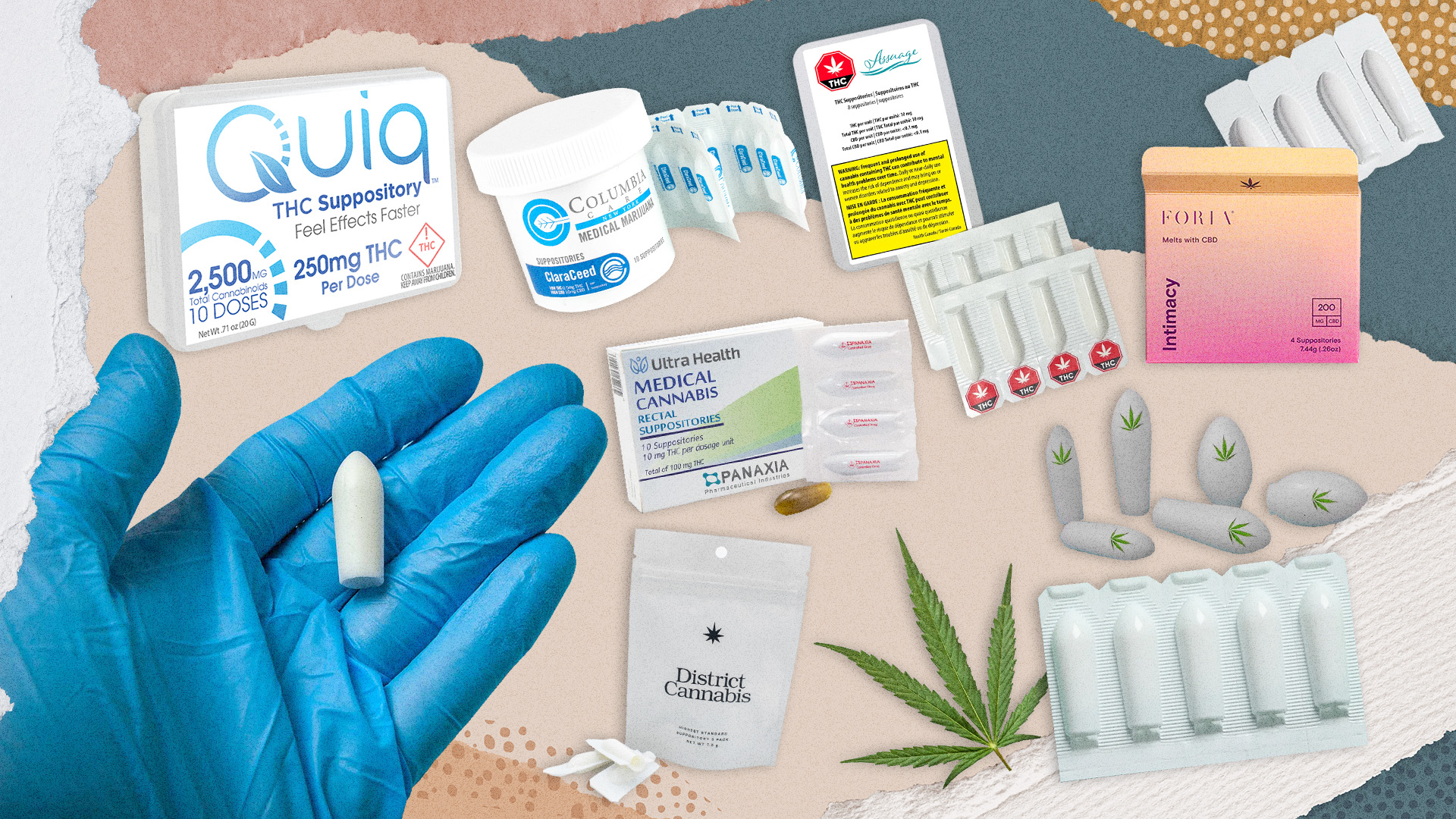
THC suppositories offer targeted therapeutic effects through rectal or vaginal insertion, providing localized relief for conditions like pelvic pain, inflammatory disorders, and chronic discomfort. Unlike oral cannabis products, suppositories deliver cannabinoids directly to surrounding tissues while bypassing first-pass liver metabolism.
This delivery method appeals to patients seeking discrete, smoke-free treatment options with potentially faster onset times than edibles. Understanding proper usage, safety considerations, and when suppositories might be preferable to other cannabis forms helps you make informed decisions about this therapeutic approach.
Both THC and cannabidiol (CBD) suppositories target localized symptoms, but they work through different mechanisms and produce distinct therapeutic effects. The choice between them depends on your specific condition, symptom severity, and tolerance for psychoactive effects.
THC suppositories primarily activate CB1 receptors in the pelvic region, providing stronger analgesic effects for severe pain conditions. CBD suppositories work through CB2 receptors and other pathways, offering anti-inflammatory benefits without psychoactivity. Many patients find combination products effective for complex conditions requiring both pain relief and inflammation reduction.
| Aspect | THC Suppositories | CBD Suppositories |
| Primary Effects | Pain relief, muscle relaxation | Anti-inflammatory, anxiety reduction |
| Onset Time | 15-30 minutes | 20-45 minutes |
| Psychoactive Effects | Mild to moderate (localized) | None |
| Best For | Severe pelvic pain, menstrual cramps, endometriosis | Inflammation, hemorrhoids, general discomfort |
| Legal Status | Medical/recreational states only | Federally legal (hemp-derived) |
| Duration | 4-8 hours | 6-12 hours |
THC suppositories work best for conditions requiring significant pain relief, such as severe menstrual cramps or endometriosis-related discomfort. Localized absorption through vaginal or rectal tissue limits systemic circulation, reducing full-body psychoactive effects, which is a significant advantage for patients seeking targeted relief. Research on whether you can absorb THC through skin suggests the mucous membrane pathway is more direct than transdermal absorption.
CBD suppositories suit patients managing inflammation-dominant conditions or those in states where THC remains restricted. The therapeutic effects typically last longer than THC, making them suitable for chronic inflammatory conditions requiring sustained relief throughout the day.
THC suppositories are cannabis-based products designed for rectal or vaginal insertion, containing concentrated tetrahydrocannabinol (THC) suspended in a suppository base like cocoa butter or coconut oil. Unlike oral cannabis products that undergo extensive liver metabolism, suppositories deliver cannabinoids directly to local tissues and the bloodstream through mucous membrane absorption.
The suppository format allows THC to bypass the digestive system entirely, providing faster onset times and higher bioavailability than edibles. Cannabis bioavailability through suppository administration typically ranges from 50-70%, significantly higher than the 10-20% bioavailability seen with oral consumption.
These products typically contain 25-100mg of THC per suppository, though dosing varies significantly between manufacturers and intended applications. The suppository base melts at body temperature, releasing cannabinoids for absorption through the highly vascularized rectal and vaginal tissues.
THC suppositories offer targeted relief for several medical conditions where localized cannabinoid delivery provides advantages over systemic administration. The direct application to pelvic tissues makes them particularly effective for gynecological and gastrointestinal conditions.
Patients with severe menstrual cramps often find suppositories more effective than oral cannabis because the THC reaches uterine tissues directly through vaginal absorption. Research suggesting THC reduces inflammatory pain indicates that localized cannabinoid application can interrupt pain signaling in pelvic nerve pathways more effectively than systemic approaches.
Primary medical applications include:
The bioavailability advantage means patients often achieve therapeutic effects with lower total cannabinoid doses compared to oral administration. Many patients choose suppositories specifically because they can maintain pain relief while avoiding the cognitive effects associated with higher systemic THC levels.
Patient experiences suggest suppositories work best for conditions involving deep, aching pain rather than sharp, acute discomfort. The onset typically begins within 20-30 minutes, with peak effects occurring around 1-2 hours post-administration.
Proper suppository insertion technique ensures maximum absorption and therapeutic benefit while minimizing discomfort. The process requires attention to hygiene, timing, and positioning for optimal results.
Clean your hands thoroughly with soap and warm water, then dry completely. Remove the suppository from refrigerated storage and allow it to reach room temperature for 2-3 minutes — cold suppositories are harder to insert and may cause discomfort.
Choose a comfortable position: lying on your side with knees drawn up, squatting, or standing with one foot elevated. Empty your bladder if using vaginal suppositories, or have a bowel movement if using rectal suppositories, ideally 30-60 minutes before insertion.
Apply a small amount of water-based lubricant to the suppository tip and insertion area if needed. Avoid oil-based lubricants with coconut oil-based suppositories, as they may dissolve the suppository prematurely.
Remain lying down for 15-20 minutes after insertion to prevent the suppository from slipping out before full absorption occurs. The suppository base will melt completely within 10-15 minutes at body temperature.
Wash your hands again with soap and water. Some patients experience mild leakage of the melted suppository base, which is normal — consider wearing a panty liner or staying near a bathroom for the first hour.
Avoid strenuous physical activity for 30-45 minutes post-insertion to allow proper absorption. Effects typically begin within 20-30 minutes, reaching peak intensity around 1-2 hours after administration.
THC suppository dosing follows different guidelines than oral cannabis products due to higher bioavailability and localized effects. Starting with conservative doses helps you find your therapeutic threshold without overshooting into uncomfortable territory.
Most suppositories contain 10-100mg of THC, with 25-50mg representing the most common therapeutic range. First-time users should start with 10-25mg to assess individual tolerance and absorption rates, as suppository effects can feel more intense than equivalent oral doses.
| Experience Level | Starting Dose | Typical Effective Range | Maximum Recommended |
| Cannabis naive | 5-10mg | 10-25mg | 25mg |
| Occasional user | 10-25mg | 25-50mg | 75mg |
| Regular user | 25-50mg | 50-100mg | 150mg |
| High tolerance | 50mg+ | 75-150mg | 200mg |
Onset typically occurs within 15-30 minutes for rectal suppositories and 20-45 minutes for vaginal suppositories. Peak effects develop around 1-2 hours post-insertion, with total duration lasting 4-8 hours depending on dose and individual metabolism.
Unlike edibles, suppository effects tend to plateau rather than intensify over time. If you don’t feel adequate relief within 2 hours, wait until the next day before increasing the dose — taking a second suppository too soon can lead to uncomfortable overconsumption.
Patients managing chronic conditions often find consistent daily dosing more effective than as-needed use. Consult with a cannabis-knowledgeable healthcare provider about developing a dosing schedule that aligns with your symptom patterns and daily routine. Getting your medical marijuana card provides access to dispensary pharmacists who can guide dosing decisions based on your specific medical needs.
THC suppositories remain less common than other cannabis products, but availability has expanded significantly in medical and recreational cannabis markets. Product selection and quality vary considerably between dispensaries and manufacturers.
Licensed dispensaries in medical cannabis states typically carry 2-5 suppository products, while recreational markets may have limited options. Call ahead to confirm availability, as many dispensaries don’t stock suppositories regularly due to lower demand compared to flower and edibles.
What to look for when shopping:
Legal access considerations:
Recreational users can purchase THC suppositories in states with adult-use cannabis laws, typically with the same purchase limits as other cannabis products. Medical patients often have access to higher-potency products and larger quantities with valid medical cannabis recommendations.
Some states allow online ordering for pickup or delivery, while others require in-person dispensary visits. Check your state’s specific regulations regarding cannabis suppository purchases and possession limits.
CBD suppositories derived from hemp are federally legal and available through online retailers, health food stores, and some pharmacies. However, THC suppositories require access to licensed cannabis dispensaries in states with medical or recreational cannabis programs.
Proper storage maintains suppository potency and prevents contamination, while safe handling practices minimize infection risk and ensure therapeutic effectiveness. THC suppositories require more careful storage than most cannabis products due to their susceptibility to temperature changes.
Storage requirements:
Shelf life and degradation signs:
Properly stored suppositories typically maintain 80-90% potency for 12-18 months. Research on THC stability in pharmaceutical preparations indicates that suppository bases protect cannabinoids better than many other formats, but temperature abuse accelerates degradation.
Replace suppositories showing color changes, unusual odors, or surface cracking. White spots or film on the surface usually indicate cocoa butter bloom, which affects appearance but not potency or safety.
Safety protocols:
When to avoid use:
Do not use THC suppositories during active vaginal or rectal infections, immediately after pelvic surgery without physician approval, or if you have severe immune system compromise. Patients taking warfarin or other blood thinners should discuss suppository use with their prescribing physician, as cannabinoids may affect clotting factors in some individuals.
Pregnant and breastfeeding patients should avoid THC suppositories due to potential fetal and infant cannabinoid exposure through systemic absorption.
THC suppositories generally produce milder systemic side effects than oral or inhaled cannabis, but localized reactions and individual sensitivities can still occur. Understanding potential adverse effects helps you recognize normal responses versus reactions requiring medical attention.
Common mild side effects:
Systemic effects requiring dose adjustment:
Higher-dose suppositories or individual sensitivity can produce systemic THC effects including dizziness, anxiety, or cognitive impairment. These effects indicate more cannabinoid absorption than intended for localized treatment.
Serious reactions requiring medical attention:
Drug interactions and contraindications:
THC can potentiate the effects of sedating medications, blood thinners, and some seizure medications. Studies on cannabinoid-drug interactions in clinical settings suggest that even localized THC absorption can affect systemic drug metabolism in sensitive individuals.
Patients with inflammatory bowel disease should use rectal suppositories cautiously, as insertion may aggravate existing tissue irritation. Similarly, patients with vaginal atrophy or severe endometriosis should start with lower doses to assess tissue tolerance.
Tolerance and dependence considerations:
Regular suppository use can lead to tolerance, requiring dose increases over time to maintain therapeutic effects. However, physical dependence appears less likely with suppository use compared to high-dose oral or inhaled cannabis, possibly due to lower overall systemic exposure.
Are you considering THC suppositories for a medical condition? A cannabis-knowledgeable physician can help determine if this delivery method suits your specific symptoms and medical history. Find a qualified medical marijuana doctor to discuss your treatment options and develop a personalized therapeutic plan.
Note: The content on this page is for informational purposes only and is not intended to be professional medical advice. Do not attempt to self-diagnose or prescribe treatment based on the information provided. Always consult a physician before making any decision on the treatment of a medical condition.
Note: Veriheal does not support illegally consuming therapeutic substances such as cannabis but acknowledges that it transpires because of the current illicit status, which we strive to change by advocating for research, legal access, and responsible consumption. Always consult a physician before attempting alternative therapies.
THC suppositories typically begin working within 15-30 minutes, with peak effects occurring 1-2 hours after insertion. The onset time depends on individual absorption rates and whether you use rectal or vaginal insertion.
THC suppositories treat localized pelvic conditions including severe menstrual cramps, endometriosis, hemorrhoids, chronic pelvic pain, and inflammatory bowel symptoms. They provide targeted relief with less systemic psychoactive effects than oral cannabis.
Licensed dispensaries in medical and recreational cannabis states carry THC suppositories, though availability varies. Call ahead to confirm stock, as many dispensaries don’t regularly carry suppositories due to lower consumer demand compared to other cannabis products.
Sign up for our newsletter

Get your medical marijuana card today
Sign up in under 5 minutes
Start By Selecting Your State