Ulcerative Colitis Symptom Relief: Can Marijuana Help?
- Cannabis and Ulcerative Colitis: Considerations to Keep in Mind
- Understanding the Different Types of Ulcerative Colitis
- What Does the Science Say About Treating Ulcerative Colitis With Cannabis?
Cannabis contains more than 500 naturally occurring compounds, including almost 150 different cannabinoids (10). The main ones being studied are cannabidiol (CBD) and delta-9-tetrahydrocannabinol (THC). These chemicals target the endocannabinoid system (ECS) in the human body. You can read more about the science behind how the ECS works here.
The main cannabinoid receptors involved in potentially managing ulcerative colitis (UC) symptoms are the CB1 and CB2 receptors. These are believed to help create the brain-gut connection. CB1 receptors affect the brain and can help relieve anxiety and other psychological components of pain (1). They can be influenced by cannabis to help calm nausea and vomiting, slow intestinal emptying, increase appetite, and reduce pain and intestinal secretions (12).
On the other hand, CB2 receptors affect immune cells and gastrointestinal epithelial cells (intestinal surface cells), but the extent of their role is still unclear. Cannabinoids affect them and can help improve the symptoms associated with the condition, such as reduced chronic pain, diarrhea, and improving quality of life for IBD patients (1).
In addition, medical marijuana can help relieve symptoms of Crohn’s disease, which is the other type of irritable bowel disease (IBD).
Cannabis and Ulcerative Colitis: Considerations to Keep in Mind
When it comes to treating ulcerative colitis, vaping or smoking medical marijuana is technically the most efficient method of use because it is easier to dose and titrate than taking edibles (1). Cannabis edibles take longer to digest and may have a delayed effect on symptom treatment. Inhaled cannabis may not be suitable for all while carrying potential long-term health risks. Also, the effects of cannabis edibles last longer without the need for smoking or vaping.
Several smaller studies have shown patients reporting improvement of symptoms using CBD and cannabis. These improvements include:
- Reduction in abdominal pain (1)
- Relief from joint pain (5)
- Improved appetite (5)
- Nausea relief (1)
- Reduced diarrhea episodes (5)
- Improved sleep (3)
- Anxiety relief (1)
- Depression relief (1)
- Weight gain (1)
It is important for patients to discuss using medical marijuana with their gastroenterologist who manages their treatment of ulcerative colitis. Animal studies have shown anti-inflammatory benefits, among others, but no actual disease modification or remission has been shown in humans. Although medical measurements of inflammation such as C-Reactive Protein (CRP) do not show improvements with the use of cannabis, surveyed patients have experienced relief from many ulcerative colitis symptoms (1).
In addition to the positive benefits of cannabis, ulcerative colitis patients must be aware of the following (4):
- Using long-term use by cannabis users is associated with an increased risk of having surgery (1)
- Increased and unknown risks for developing babies during pregnancy, during breastfeeding, and for the elderly
- Impaired short-term memory
- Impaired coordination and judgment
- Increase in anxiety
Understanding the Different Types of Ulcerative Colitis
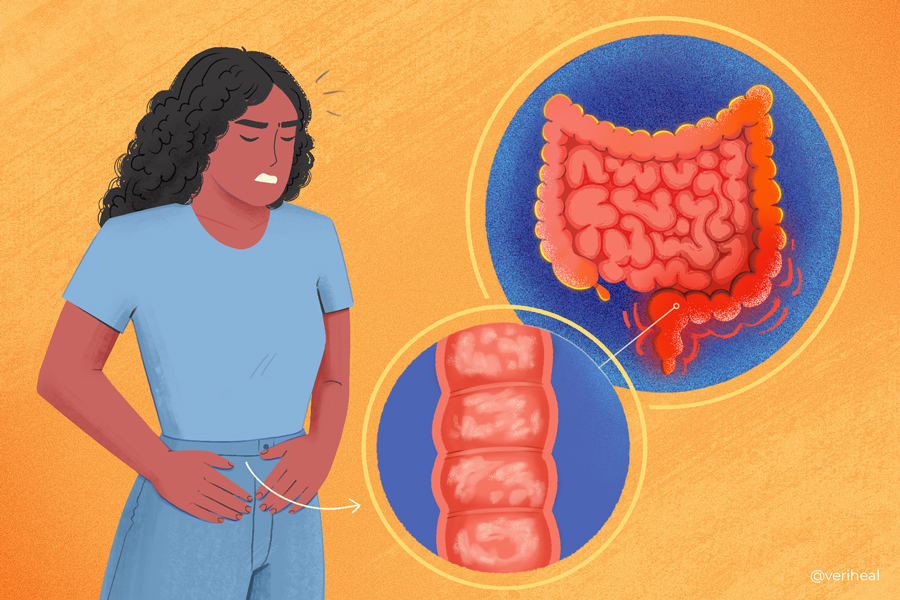
Ulcerative colitis is considered an irritable bowel disease (IBD) much like Crohn’s disease. When your body fights off sickness, the body sends white blood cells of the immune system to attack cells in different areas of your body to heal you. In UC, the body sends white blood cells to attack the lining of the large intestine, resulting in ulcers along the lining of the large intestine (5). Therefore, the condition is considered an autoimmune disorder.
According to the Crohn’s and Colitis Foundation, there are three types of ulcerative colitis that are discussed below.
Ulcerative Proctitis is where the inflammation is concentrated in the rectum, the last segment of the large intestine. It typically results in less than six inches of the rectum being inflamed and thankfully doesn’t cause an increased risk of cancer (8). Symptoms include (8):
- Urgent bowel movements
- Rectal pain
- Rectal bleeding
Left-sided Colitis is inflammation that begins in the rectum near the sigmoid portion of the large intestine. This type of colitis extends to the bend in the colon close to the spleen and has the following symptoms (8):
- Loss of appetite
- Weight loss
- Bloody diarrhea
- Left-sided abdominal pain
Extensive Colitis affects the entire large intestine and has the following symptoms (8):
- Loss of appetite
- Bloody diarrhea
- Weight loss
- Generalized abdominal pain
What Does the Science Say About Treating Ulcerative Colitis With Cannabis?
There have been several studies focusing on treating IBD with medical marijuana and other cannabinoids that overall tend to have mixed results. Often, patients report positive changes in symptoms, but inflammatory biomarkers and clinical evidence of IBD remission are typically not appreciable. Patients typically report improvements in general well-being, abdominal pain, diarrhea, and increases in appetite (9).
In a small research study out of Israel, participants with ulcerative colitis were provided with two 0.5 g cigarettes containing cannabis or a placebo. Patients were assessed after 8 weeks of treatment with an endoscopy and laboratory tests. Participants who received the cannabis cigarettes had their Mayo endoscopic scores averages decreased by one point and their CRP scores increased; however, these changes are not statistically significant (7).
These smaller studies are laying important groundwork for patients with UC due to increased interest, because of cannabis legalization as well as ongoing research about the endocannabinoid system (12). The ECS has been linked to intestinal inflammation, nausea and vomiting, gastrointestinal motility, and visceral pain perception (1).
A review of two studies focusing on cannabinoids and synthetic or natural cannabinoid derivative use in UC shows us that more research in the area is warranted and that the effects of such treatments are still clinically unknown. One study focused on smoking cannabis cigarettes while the other study analyzed CBD capsule use. These studies follow the same trend as other cannabis studies on IBD in that clinical markers of remission have not been seen and that larger-scale studies are needed to get a clearer picture of using the cannabis plant for this condition (11).
Note: Veriheal does not intend to give this as professional medical advice. Do not attempt to self-diagnose, or prescribe treatment options based on the information provided on this page. Always consult a physician before making any decision on the treatment of a medical condition.
1. Arun Swaminath, MD, Eric P Berlin, JD, Adam Cheifetz, MD, Ed Hoffenberg, MD, Jami Kinnucan, MD, Laura Wingate, Sarah Buchanan, Nada Zmeter, MD, David T Rubin, MD, The Role of Cannabis in the Management of Inflammatory Bowel Disease: A Review of Clinical, Scientific, and Regulatory Information: Commissioned by the Crohn’s and Colitis Foundation, Inflammatory Bowel Diseases, Volume 25, Issue 3, March 2019, Pages 427–435, https://academic.oup.com/ibdjournal/article/25/3/427/5144402.
2. Bauer MD, B. (2018, October 10). How the Endocannabinoid System Connects Your Gut and Your Brain. Retrieved November 15, 2020, from https://www.thorne.com/take-5-daily/article/how-the-endocannabinoid-system-connects-your-gut-and-your-brain.
3. Foundation Position Statement: Medical cannabis [PDF]. (2019, March). New York: Crohn’s & Colitis Foundation. https://www.crohnscolitisfoundation.org/sites/default/files/legacy/resources/MedicalCannabis-Position-2018-Final-002.pdf.
4. Medical Cannabis. (2020). Retrieved November 15, 2020, from https://www.crohnscolitisfoundation.org/complementary-medicine/medical-cannabis.
5. Overview of Ulcerative Colitis. (2020). Retrieved November 15, 2020, from https://www.crohnscolitisfoundation.org/what-is-ulcerative-colitis/overview.
6. Sawani, J. (2020, February 11). Cannabis for Treating IBD: Hope or Hype? Retrieved November 15, 2020, from https://healthblog.uofmhealth.org/digestive-health/cannabis-for-treating-ibd-hope-or-hype.
7. T Naftali, L Bar Lev Schlieder, F Sklerovsky Benjaminov, I Lish, J Hirsch, F M Konikoff, P398 Cannabis induces clinical and endoscopic improvement in moderately active ulcerative colitis (UC), Journal of Crohn’s and Colitis, Volume 12, Issue supplement_1, February 2018, Page S306, https://academic.oup.com/ecco-jcc/article/12/supplement_1/S306/4808102.
8. Types of Ulcerative Colitis. (2020). Retrieved November 15, 2020, from https://www.crohnscolitisfoundation.org/what-is-ulcerative-colitis/types-of-ulcerative-colitis.
9. Doeve, B. H., van de Meeberg, M. M., van Schaik, F., & Fidder, H. H. (2020). A Systematic Review With Meta-Analysis of the Efficacy of Cannabis and Cannabinoids for Inflammatory Bowel Disease: What Can We Learn From Randomized and Nonrandomized Studies?. Journal of clinical gastroenterology, 10.1097/MCG.0000000000001393. Advance online publication. https://pubmed.ncbi.nlm.nih.gov/32675631/.
10. Hanuš, L., Meyer, S., Muñoz, E., Taglialatela-Scafati, O., & Appendino, G. (2016). Phytocannabinoids: A Unified critical inventory. Natural Product Reports, 33(12), 1357-1392. https://pubs.rsc.org/en/content/articlelanding/2016/NP/C6NP00074F#!divAbstract.
11. Kafil, T. S., Nguyen, T. M., MacDonald, J. K., & Chande, N. (2018). Cannabis for the treatment of ulcerative colitis. The Cochrane database of systematic reviews, 11(11), CD012954. https://pubmed.ncbi.nlm.nih.gov/30406638/.
12. Perisetti, A., Rimu, A. H., Khan, S. A., Bansal, P., & Goyal, H. (2020). Role of cannabis in inflammatory bowel diseases. Annals of gastroenterology, 33(2), 134–144. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7049239/.